Pseudomonas Skin Infection: What It Looks Like and How It Is Treated
A pseudomonas skin infection is caused by Pseudomonas aeruginosa, a gram-negative bacterium that thrives in moist environments and opportunistically infects skin with compromised integrity. While healthy intact skin rarely becomes infected with this pathogen, wounds, burns, surgical sites, and skin folds provide entry points where the bacteria can take hold. Understanding pseudomonas skin infection pictures in terms of what visual patterns to look for, alongside the related topic of e coli skin infection, helps people recognize bacterial skin conditions that need medical attention rather than home care alone.
Pseudomonas aeruginosa skin infection is particularly concerning in hospital settings and for people who use hot tubs or pools, where the organism can survive in improperly chlorinated water. E coli on skin is a separate but related concern, most often arising from fecal contamination and affecting wounds or skin areas near mucous membranes. Both organisms require proper medical diagnosis and targeted antibiotic treatment.
What Does a Pseudomonas Skin Infection Look Like?
Hot Tub Folliculitis
One of the most recognizable presentations of pseudomonal skin infection is hot tub folliculitis. It produces itchy, red, follicle-centered pustules or papules that appear within 12 to 72 hours after contact with contaminated water. The rash typically affects areas covered by a swimsuit and resolves on its own in mild cases within one to two weeks once exposure to the source is eliminated. Severe or widespread cases benefit from oral antibiotics targeting Pseudomonas, such as ciprofloxacin.
Wound Infections and Ecthyma Gangrenosum
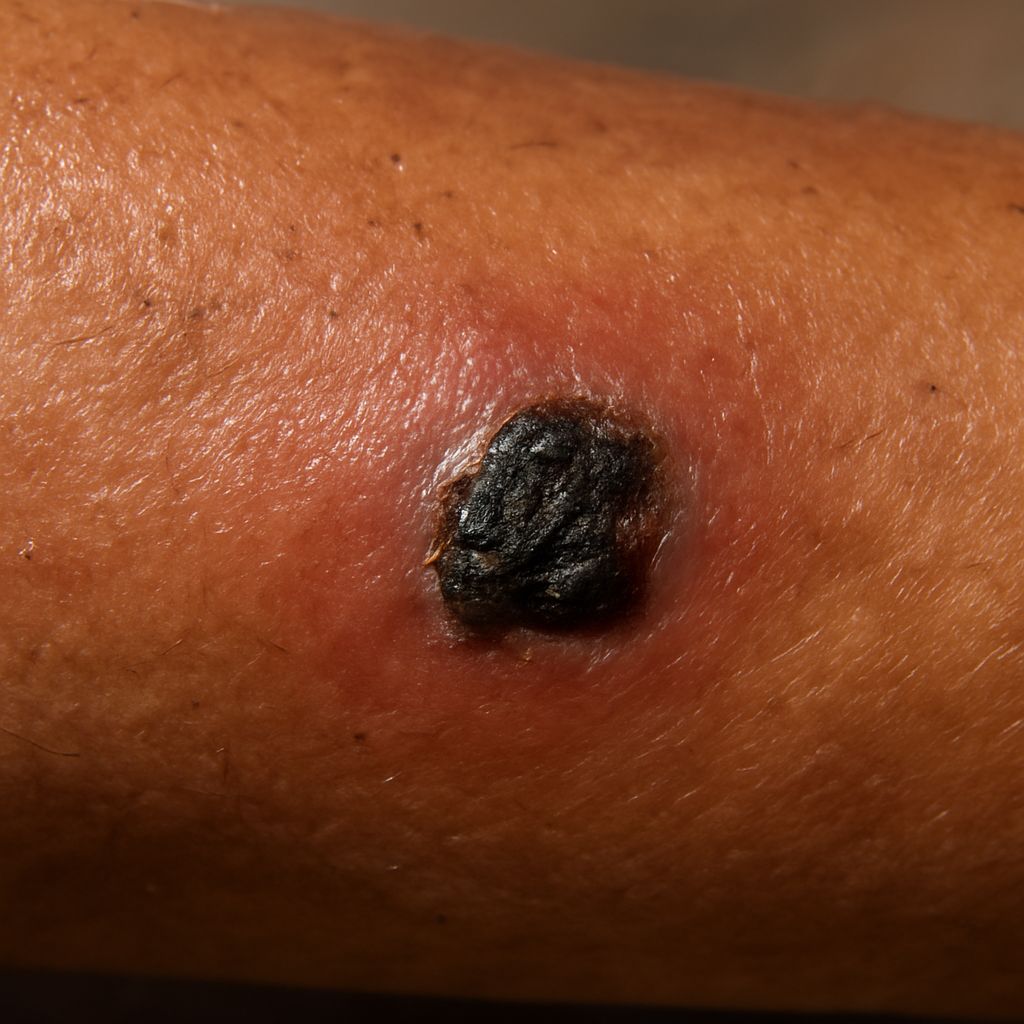
Pseudomonas aeruginosa infections in chronic wounds or in immunocompromised patients can produce a distinctive blue-green discoloration due to pyocyanin pigment secreted by the bacteria. A more serious form, ecthyma gangrenosum, presents as rapidly evolving hemorrhagic blisters that turn black and necrotic. This presentation typically occurs in severely ill patients with bacteremia and represents a dermatological emergency requiring intravenous antibiotics and urgent hospitalization.
Risk Factors for Pseudomonas Aeruginosa Skin Infection
People at elevated risk for pseudomonas aeruginosa skin infections include those with burn injuries, diabetic foot ulcers, pressure injuries, surgical wounds, or those undergoing chemotherapy that suppresses immune function. Ear infections in swimmers, known as swimmer’s ear, are another common pseudomonas presentation. The pathogen is naturally resistant to many common antibiotics, which is why culture and sensitivity testing before initiating treatment is important for appropriate antibiotic selection.
E. Coli Skin Infection: How It Differs from Pseudomonas
How E. Coli Reaches the Skin
E coli skin infections are less common than pseudomonas but occur in similar clinical contexts. E coli on skin most frequently causes cellulitis or wound infections, particularly in areas near the perineum, abdomen following bowel surgery, or legs in patients with venous insufficiency. The mechanism is typically direct contamination from the gastrointestinal tract or environment rather than water-borne exposure as seen with pseudomonas.
Signs of E. Coli Cellulitis
An e coli skin infection presenting as cellulitis shows warmth, redness, swelling, and tenderness in the affected area. Unlike pseudomonas, e coli does not produce the characteristic blue-green pigment or follicular pattern. The skin may appear uniformly red and feel hot, with edges that spread if left untreated. Fever and elevated white blood cell count are common systemic signs that indicate the infection has penetrated beyond the skin surface.
Diagnosis and Treatment
Accurate diagnosis of either pseudomonas or e coli skin infections requires a wound culture or swab sent to a microbiology laboratory. Visual inspection alone cannot reliably distinguish between bacterial species. Once the organism and its antibiotic sensitivities are identified, a clinician prescribes targeted treatment. Pseudomonas is typically treated with anti-pseudomonal penicillins, fluoroquinolones, or aminoglycosides depending on severity. E coli skin infections generally respond to beta-lactam antibiotics, though resistance rates vary by geographic region and require culture guidance.
Prevention Strategies
Preventing pseudomonas-related skin infections means avoiding contact with improperly maintained hot tubs, pools, or whirlpools, and keeping skin wounds covered and clean. For hospital patients, strict wound care protocols and infection control practices significantly reduce transmission risk. Preventing e coli skin infections centers on thorough hand hygiene, proper wound care, and maintaining skin integrity, particularly in high-risk individuals such as diabetic patients or those with chronic venous disease.
Pro tips recap: Any skin wound with blue-green discoloration, expanding redness, or failure to heal after standard wound care deserves prompt medical evaluation for bacterial infection. Never attempt to treat suspected pseudomonas or e coli skin infections with over-the-counter antibiotic creams alone, as neither organism responds adequately without systemic antibiotics in most cases. Early culture-guided treatment prevents progression to serious systemic infection.






Leave a Reply